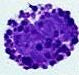
Human Normal Peripheral Blood Basophils
A basophil is a type of white blood cell and the least common type of granulocyte, normally making up approximately 0.5 to 3 percent of the peripheral blood leukocytes. However, they are the largest type of granulocyte that has granules (small particles) with enzymes that are released during allergic reactions including anaphylaxis, asthma, atopic dermatitis and hay fever.
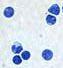
Basophil's name comes from the fact that they are basophilic, i.e., they are susceptible to be stained by basic dyes, such as haematoxylin (most common dye), as shown in the following picture.
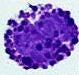
Basophils perform phagocytosis (cell eating), produce histamine and serotonin that induce inflammation, and heparin that prevents blood clotting. It used to be thought that basophils that have migrated from blood into their resident tissues (connective tissue) are known as mast cells, but this is no longer thought to be the case.
Our Human Normal Peripheral Blood Basophils are isolated from peripheral blood mononuclear cells by indirect immunomagnetic selection. All peripheral blood is collected in acid-citrate-dextrose formula A (ACDA) by leukapheresis from fully consented IRB approved donors that are tested negative for HIV, HBV, and HCV.
Structure
Basophils contain large cytoplasmic granules which obscure the cell nucleus under the microscope when stained. However, when unstained, the nucleus is visible and it usually has two lobes. The mast cell, another granulocyte, is similar in appearance and function. Both cell types store histamine, a chemical that is secreted by the cells when stimulated. However, they arise from different branches of hematopoiesis, and mast cells usually do not circulate in the blood stream, but instead are located in connective tissue. Like all circulating granulocytes, basophils can be recruited out of the blood into a tissue when needed.
Function
Basophils appear in many specific kinds of inflammatory reactions, particularly those that cause allergic symptoms. Basophils contain anticoagulant heparin, which prevents blood from clotting too quickly. They also contain the vasodilator histamine, which promotes blood flow to tissues. They can be found in unusually high numbers at sites of ectoparasite infection, e.g., ticks. Like eosinophils, basophils play a role in both parasitic infections and allergies. They are found in tissues where allergic reactions are occurring and probably contribute to the severity of these reactions. Basophils have protein receptors on their cell surface that bind IgE, an immunoglobulin involved in macroparasite defense and allergy. It is the bound IgE antibody that confers a selective response of these cells to environmental substances, for example, pollen proteins or helminth antigens. Recent studies in mice suggest that basophils may also regulate the behavior of T cells and mediate the magnitude of the secondary immune response.
Secretions
Basophils arise and mature in bone marrow. When activated, basophils degranulate to release histamine, proteoglycans (e.g. heparin and chondroitin), and proteolytic enzymes (e.g. elastase and lysophospholipase). They also secrete lipid mediators like leukotrienes (LTD-4), and several cytokines. Histamine and proteoglycans are pre-stored in the cell's granules while the other secreted substances are newly generated. Each of these substances contributes to inflammation. Recent evidence suggests that basophils are an important source of the cytokine, interleukin-4, perhaps more important than T cells. Interleukin-4 is considered one of the critical cytokines in the development of allergies and the production of IgE antibody by the immune system. There are other substances that can activate basophils to secrete which suggests that these cells have other roles in inflammation.
The degranulation of basophils can be investigated in vitro by using flow cytometry and the so-called basophil-activation-test (BAT). Especially, in the diagnosis of allergies including of drug reactions (e.g. induced by contrast medium), the BAT is of great impact.
Basopenia (a low basophil count) is difficult to demonstrate as the normal basophil count is so low; it has been reported in association with autoimmune urticaria[13] (a chronic itching condition). Basophilia is also uncommon but may be seen in some forms of leukaemia or lymphoma.